Case Report 
 Creative Commons, CC-BY
Creative Commons, CC-BY
Quality of Life in Patients with Low Back Pain After Chiropractic Instrumental Manipulation–A Case Study
*Corresponding author:Maria Eduarda de Souza Melo Oliveira, Policlínica Piquet Carneiro, Universidade do Estado do Rio de Janeiro (UERJ), Avenida Marechal Rondon 381 - São Francisco Xavier, Rio de Janeiro-RJ, 20950-003, Brazil.
Received:June 28, 2022; Published:July 08, 2022
DOI: 10.34297/AJBSR.2022.16.002272
Abstract
Objective: To analyze the quality of life (QoL) of patients with nonspecific low back pain (NLBP) after Chiropractic Instrumental
Manipulation (CIM).
Methods: Three patients with NLBP underwent an instrumental chiropractic application with force maximum strength in the
region with dysfunction, for four weeks. The tests performed before and after the intervention were
a) Visual Analogue Pain Scale (VAS),
b) SF-36 Quality of Life Questionnaire,
c) Womac Questionnaire, and
d) Lequesne Algofunctional Assessment.
Results: In all three patients evaluated, through the questionnaires, pain, and QoL improved. Conclusion: The CIM has proven to
be an effective and safe treatment intervention for patients with NLBP, in improving Qol.
Keywords: A case study, Chiropractic instrumental manipulation, Low Back Pain, Quality of life
Introduction
There are two types of low back pain (LBP): Specific, when there is a determinant cause, or non-specific, which is pain not attributed to a recognizable pathology [1]. Up to 90% of patients with LBP, cannot make a specific diagnosis and therefore patients are classified as having ‘non-specific’ low back pain (NLBP) [2]. The pain caused by NLBP produces a functional incapacity in the lives of these patients [3], generating a negative effect on their quality of life (QoL) [4]. According to the World Health Organization (WHO) [5], QoL is “the individual’s perception of their insertion in life, in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns”. LBP is the leading cause of global disability and a common reason for work absenteeism lost productivity and looking for medical care [6,7].
The treatment of NLBP focuses on pain reduction and its consequences [8]. Pain management approaches vary widely [9]. Non-steroidal anti-inflammatory drugs, opioids, neurotropic drugs, or steroid injections and surgery are the main tools used in treatment [10]. Another approach method for the treatment of low back pain is Chiropractic Instrumental Manipulation. This manipulation uses an instrument able to safely, and punctually reduce dysfunctions. This therapy based on the Leg Check (leg length check) to identify subluxations or dysfunctions [11]. The chiropractic instrumental method uses three tests in its protocol to find the subluxation, Pressure test, stress test, and isolation test. After identifying the location, and how the subluxation occurs, the adjustment will be performed [12].
This instrument produces a gentle impulse (vibration or micro impulse) that sends information to the nervous system, triggering a rebalancing process, restoring a normal and painless range of joints, and consequently relaxing all associated muscles [13]. Thus, specific adjustments promote the activation of micro-movements and unlock the joints through small impacts on specific points [11]. It is a technique indicated for the treatment of biomechanical restrictions, postural disorders, acute and chronic pain [10,12]. The chiropractic instrumental manipulation intended for everyone, from pediatrics to geriatrics, without forgetting sports pathologies.
The chiropractic instrumental sessions brought benefits to
patients safely and quickly. Several questionnaires and scales used
to assess the quality of life and pain of patients, but in this study, we
used to assess patients with NBLP before and after the chiropractic
instrumental manipulation:
a) SF-36 Quality of Life Questionnaire [14].
b) Womac Questionnaire [15].
c) Visual Analogue Pain Scale (VAS) [16].
d) Lequesne Algofunctional Assessment [17].
The SF-36 Quality of Life Questionnaire is a generic instrument whose conceptual basis is “health-related quality of life”. This instrument represented by 36 questions divided into eight domains: physical functioning, role physical, pain, general health, vitality, role social, role emotional and mental health. Items scored by a Likert scale. All items of SF-36 used to score the eight domains, except for item 2, which refers to a self-report of health transition. Each item contributes to only one domain. The WOMAC questionnaire is an instrument developed in 19825, to be used in patients with osteoarthritis. It contains 24 questions grouped into three dimensions: five to assess pain, two for joint stiffness and 17 for physical capacity. The WOMAC score can range from 0 to 96 and be divided into three different scores: pain (0-20), joint stiffness (0- 8), and physical capacity (0-68).
The higher the score, the worse the dimension evaluated. Assesses the patient’s pain and quality of life. The visual analog scale (VAS) is a validated, subjective measure for acute and chronic pain. Scores recorded by making a handwritten mark on a 10-cm line that represents a continuum between “no pain” and “worst pain.” Lequesne Algofunctional Assessment is composed of 11 questions about pain, discomfort, and function, being six questions about pain and discomfort (one of these being different for the knee and the other for the hip), one about walking distance and four different about the hip or knee about activities of daily living. Scores range from 0 to 24 (non-impaired to extremely severe, respectively). The objective is to analyze the QoL results of patients with NLBP, before and after chiropractic instrumental manipulation.
Case Presentation
That study was a 4-week with three patients (62±43,33 years) with NLBP selected to assess the effect of CIM on QoL and pain. This study was carried out from November 2021 to February 2022, performed by physiotherapists at the LIVTA Institute in São Paulo, Brazil. Participants were sedentary and instructed to continue their normal daily activities and medications during the investigation.
Inclusion Criteria
Patients of both genders aged 40 years or over, diagnosed with NLBP.
Exclusion Criteria
Post-surgical patients with arthrodesis in the lumbar spine, neurological patients, recent fractures, and bone pathologies (tumors and diseases osteometabolic).
Primary Results
In this investigation, the findings related to the parameters evaluated before and after a four-week protocol involving chiropractic instrumental manipulation considered. Before the first session, the results performed in sequence, answering the questionnaires and the scales. After the last session, the evaluations carried out in the same way.
Intervention
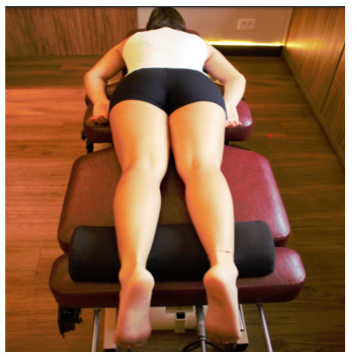
Before the first session of the CIM program, patients were instructed to continue their normal daily activities and medicine during the investigation. All patients confirmed at the end of the study that the instructions were followed. The protocol was carried out in 6 weeks (12 sessions). In the first session, we analyzed the clinical examination, the anamnesis, and the patient’s history, palpated the region that presented the functional limitation and the pain, and checked the complementary exams. After this phase, we started the execution of the Chiropractic instrumental protocol. This protocol is performed through “Leg Check”, which will indicate where to adjust, when to adjust and when not to adjust. The patient answered the questionnaires (SF-3614, Womarc15, EVA16, and Lequesne Algofunctional Assessment 17, and was positioned in a prone position on a stretcher with an orifice and placing his bare feet outside the stretcher with the support of the positioning roller under the distal region of the tibia (Figure 1).
In table 1, we show the chiropractic instrumental protocol for
adjustments in the low back region subluxations. This protocol
consists of four steps
I. Perform pressure and isolation tests to assess joint function
and confirm the diagnosis.
II. Perform passive stress tests to identify the subluxation in the
lumbar region.
III. We isolated the region and side of the subluxation to be
adjusted.
IV. We perform the correction test to confirm the direction of
adjustment. This subluxation adjustment was done with an
instrument graduated at strength 4 (16Kgf).
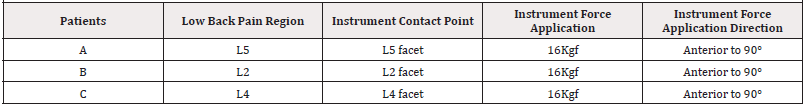
In the CIM, three patients with NBLP were selected according to the inclusion criteria. In this work, patients are identified by a letter (A, B, and C). Table 2 shows the protocol used for each patient. We had 1 patient with limitations and pain in the L5 region, 1 in the L2 region and 1 in the L4 region. The force used in the instrument chiropractic was 16 Kgf and the application site was on the facet, anatomical process of the lumbar vertebrae. The direction of application force was anterior to 900 in patients (Table 3).
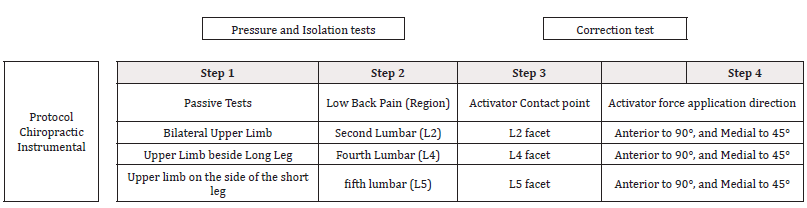

Table 1: Protocol Instrumental Chiropractic: Tests, Region of patient complaint, Instrument contact point in their lower back, force application direction.
Results
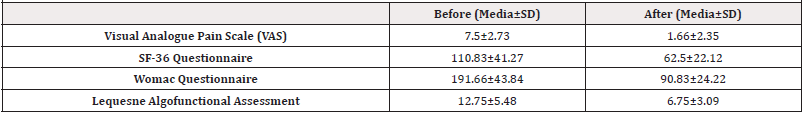
The results before the first and after the last session of chiropractic instrumental manipulation protocol with questionnaires, and scales are presented in Table 4, and the anthropometric characteristics of the participants are shown in Table 3. This study demonstrated the benefits of chiropractic instrumental manipulation in NLBP patients. With 4 sessions in four weeks of protocol, we observed an improvement in the pain and QoL. In all results, there was a decrease in pain and an increase in the patients’ quality of life. On the VAS pain scale, the decrease was from 7.5±2.73 to 1.66±2.35. In the SF-36 questionnaire that assesses the impact of the pathology on the patient’s life, it changed from 110.83±41.27 to 62.5±22.12, meaning an increase in QoL. In the WOMAC questionnaire, and in the Lequesne Algofunctional Assessment, observed the same scenario positive results (191.66±43.84 to 90.83±24.22) and, in the WOMAC, (14.33±4.38 to 14.33±4.38)
Discussion
Although this article is just a case study with three patients and the chiropractic instrumental manipulation technique is still very controversial, the results have shown a great short-term benefit for patients who have been suffering from pain that reduces their ability to deal with the everyday tasks, especially at work. Many articles such as [18,19] corroborate this approach. I believe that we need more studies, with a greater number of participants so that we can have a formed opinion about this technique.
Conclusion
Instrumental chiropractic manipulation proved to be an effective and safe therapy for this group of patients with non-specific low back pain, reducing pain in a short period and improving the quality of life of these patients. It is important to consider the need to carry out studies with a high level of evidence on the outcome analyzed.
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
- Koes BW, Van Tulder M, Lin CW, Luciana G Macedo, James Mc Auley, et al. (2010) An updated overview of clinical guidelines for the management of non-specific low back pain in primary care. Eur Spine J 19(12):2075-2094.
- Owen PJ, Miller CT, Mundell NL, Simone JJ M Verswijveren, Scott D Tagliaferri, et al. (2020) Which specific modes of exercise training are most effective for treating low back pain? Network meta-analysis. Br J Sports Med 54(21): 1279-1287.
- Hayden JA, Wilson MN, Stewart S (2020) Chronic Low Back Pain IPD Meta-Analysis Group. Exercise treatment effect modifiers in persistent low back pain: an individual participant data meta-analysis of 3514 participants from 27 randomised controlled trials. Br J Sports Med 54(21): 1277-1278.
- Morlion B (2013) Chronic low back pain: pharmacological, interventional and surgical strategies. Nat Rev Neurol 9(8): 462-473.
- T (1998) Development of the World Health Organization WHOQOL-BREF Quality of Life Assessment. The WHOQOL Group . Psychological Medicine 28(3): 551-558.
- Driscoll T, Jacklyn G, Orchard J, E Passmore, T Vos, G Freedman, et al. (2014) The global burden of occupationally related low back pain: estimates from the Global Burden of Disease 2010 study. Ann Rheum Dis 73(6): 975-981.
- GBD 2017 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392(10159): 1789-1858.
- Safiri S, Kolahi AA, Hoy D (2017) Global, regional, and national burden of neck pain in the general population, 1990-2017: systematic analysis of the Global Burden of Disease Study 2017. BMJ.
- Treleaven J (2008) Sensorimotor disturbances in neck disorders affecting postural stability, head and eye movement control. Man Ther 13(1): 2-11.
- Zhang M, Du G, Liu C, Wei Li, Jiayu Yang, et al. (2021) Efficacy and safety of Shi-style cervical manipulation therapy for treating acute and sub-acute neck pain: study protocol for a randomized controlled trial. Trials 22(1): 123.
- Fuhr AW (1997) Activator Methods Chiropractic Technique; St. Louis: Mosby p.92
- Fuhr AW (2010) Activator Methods International Ltd.
- Soulier F (2010) D Equilibration Neuro Musculaire; niveau I.
- Ciconelli RM, Ferraz MB, Santos, Wilton (1999) Tradução para língua portuguesa e validação do questionário genérico de avaliação de qualidade de vida SF-36 (Brasil SF-36)/Brazilian- Portuguese version of the SF-36. A reliable and valid quality of life outcome. Rev Bras Reumatol 39(3): 143-150.
- Gogtay NJ, Thatte UM, Dasgupta B, S Deshpande (2013) Use of the WOMAC questionnaire in Mumbai and the challenges of translation and cross-cultural adaptation. Indian J Med Ethics 10(1): 33-35.
- Delgado DA, Lambert BS, Boutris N, Patrick C McCulloch, Andrew B Robbins, et al. (2018) Validation of Digital Visual Analog Scale Pain Scoring with a Traditional Paper-based Visual Analog Scale in Adults. J Am Acad Orthop Surg Glob Res Rev 2(3): e088.
- Faucher M, Poiraudeau S, Lefevre-Colau MM, F Rannou, J Fermanian, et al. (2002) Algo-functional assessment of knee osteoarthritis: comparison of the test-retest reliability and construct validity of the WOMAC and Lequesne indexes. Osteoarthritis Cartilage 10(8): 602-610.
- Schneider M, Haas M, Glick R, Joel Stevans, Doug Landsittel, et al. (2015) Comparison of spinal manipulation methods and usual medical care for acute and sub-acute low back pain: a randomized clinical trial. Spine (Phila Pa 1976) 40(4): 209-217.
- Huggins T, Boras AL, Gleberzon BJ (2012) Clinical effectiveness of the Activator adjusting instrument in the management of musculoskeletal disorders: a systematic review of the literature. J Can Chiropr Assoc 56(1): 49-57.




 We use cookies to ensure you get the best experience on our website.
We use cookies to ensure you get the best experience on our website.